Health care workers on the front lines of the COVID-19 pandemic have handled an unprecedented strain on medical supply chains and human resources, testing and tending to patients, educating the public, and implementing and adapting to new safety protocols for themselves and their patients.
They were alerted early to the coronavirus news in China and began steps to protect facilities and staff and prepare for a potential surge in patients—to date keeping capacity well ahead of demand.
Preparation, testing and treatment
With a new, highly contagious and not-fully-understood virus to battle, safety has been a primary concern for health care officials.
Dr. Mark F. Newman, the University of Kentucky’s executive vice president for health affairs, said there are more than 9,200 Kentucky-based employees at UK HealthCare, the clinical arm of UK that includes three hospitals and more than 120 ambulatory clinics.
In mid-January, Newman said, UK Healthcare began screening patients who’d traveled to China over the holidays and had returned to UK’s campus.
“Since then, our Infection Prevention and Control team has worked with campus colleagues, city and state officials and throughout the health care enterprise to continually update procedures and protocols to keep patients, employees and students safe,” he said.
These actions included providing telecare options at nearly all affiliated clinics as well as drive-thru testing for health care employees and in-house COVID-19 testing since March 21. In the first four weeks of testing, the lab completed nearly 3,000 tests.
To address additional hospital capacity needs, UK Healthcare announced in early April that the UK football team’s on-campus practice facility, Nutter Field House, would be transformed into a 400-bed field hospital, which was completed by April 20.
- IT’S FREE | Sign up for The Lane Report email business newsletter. Receive breaking Kentucky business news and updates daily. Click here to sign up
Another field hospital with a capacity for 2,000 beds went up at the Kentucky Fair & Exposition Center in Louisville, staffed by the Kentucky National Guard, should hospitals run short on space for new COVID-19 patients.
UofL Health CEO Tom Miller started hearing rumblings about COVID-19 in January, and by February many preparations were underway. UofL Health operates five hospitals and four medical centers along with more than 200 physician practice locations and the Frazier Rehab Center and James Graham Brown Cancer Center.
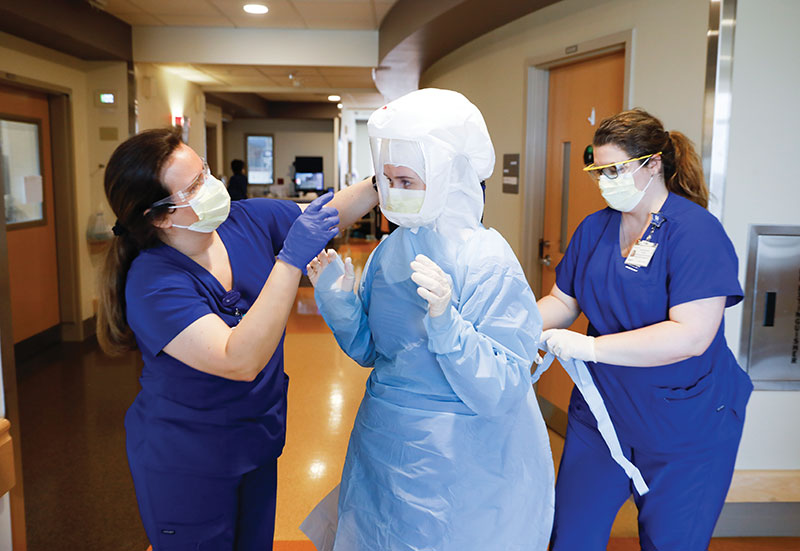
The first priority was to protect the health of the medical staff so they’d be able to take care of patients, in part making sure they had enough personal protective equipment (PPE), which was a challenge. By working outside normal purchasing vendors, they made good headway.
Visitation was restricted and most waiting rooms closed as new processes enabled patients to wait in their vehicles until they were called in for medical appointments. Protective masks were required for staffers and visitors, handwashing stations were prominently placed throughout facilities, and temperature-taking protocols were established for visitors and staff.
“We consider this (pandemic) a disaster situation so we opened up an incident command,” Miller said, explaining the group meets regularly to discuss ICU bed availability, patient volumes, PPE needs, exposure reduction methods and best practices for helping patients.
About 700 UofL Health staff began working from home. With elective surgeries put on hold, fewer personnel were needed on medical floors, so about 200 others volunteered to stay home unless recalled to duty, a boon for those with children out of school.
UofL Health facilities still had plenty of available beds in late April. Normally there are 900 inpatients per day throughout the network; as elective procedures were halted, the census dropped to about 700 daily, providing additional capacity if needed.
Saint Joseph Health CEO Bruce Tassin, which leads a health care system with 135 locations in 20 Kentucky counties, acknowledged that the suspension of elective procedures was challenging for many non-COVID patients.
“The COVID-19 pandemic has impacted all of us, and it has been difficult for some patients as we paused services such as diagnostic and radiology testing, nonurgent procedures and elective surgeries,” said Tassin. However, he added, “We appreciate the governor’s thoughtful and safety-focused decision, and have taken a number of steps to reinforce the health and safety of patients utilizing our services, as well as for our staff members.”
With about 17,000 Kentucky-based employees, Baptist Health began preparing for the impacts of COVID-19 weeks before Kentucky reported its first case, according to Public Relations Manager Kit Fullenlove.
“A core team began meeting daily to make sure we had resources in place, such as personal protective equipment (PPE), staffing plans and to begin facility surge planning for all our hospitals,” she said.
Planning commenced with state and local governments as well as other health systems and key providers such as EMS. By April 8, Baptist Health had tested more than 4,000 people with symptoms similar to COVID-19, with about 10% positive cases. Meanwhile, existing telecommuting infrastructure was expanded to allow up to 3,800 employees to work from home.
At Pikeville Medical Center, CEO Donovan Blackburn and Chief Medical Officer Dr. Aaron Crum said their hospital network, which encompasses 3,000 employees among its 45 different facilities, was well poised for the COVID-19 battle.
Two infectious disease doctors and a director of infectious disease are on staff, and enough “negative-pressure rooms”—which contain airflow and isolate patients with contagious conditions—for 40 patients at once, with additional expansion capabilities.
The hospital became home to a Highly Infectious Disease Unit in 2015, part of an effort to prevent a widespread Ebola outbreak as had occurred in Africa.
“We’re very fortunate that we were essentially very prepared in large part,” Crum said.
In Northern Kentucky, Edgewood-based St. Elizabeth Healthcare operates five facilities and many private physician practices, in all employing about 9,000. CEO Garren Colvin said an infectious disease team has been constantly planning for a major local outbreak of some form while monitoring past Ebola, swine flu, SARS and others for more than 10 years.
“We always had a team in place for what we thought was coming,” he said.
Two wings of the hospital have been transformed into negative pressure rooms. Though PPE remains a concern, community donations have helped, and overall, he said, supply volumes and staffing levels are stable. As a contingency, St. Elizabeth Healthcare officials have been working with the Kentucky Board of Nursing to get new graduates licensed quickly, and PRN staff have been asked whether they could work more hours if needed.
Collaboration, innovation is critical
Just as medical facilities have had to quickly adapt operations to the “new normal” of the COVID-19 era, so have the operations of Kentucky-based insurers and other providers.
Louisville-based insurance company Humana Inc. has about 12,000 Kentucky-based employees, many of whom have always telecommuted, said Humana Corporate Communications Lead Kate Marx. Employees typically work scheduled hours from home, appearing in-office for occasional team meetings or other events.
“Our work-at-home policy has been very successful over a number of years and has resulted in higher levels of performance and employee engagement,” Marx said. “Our success is attributable to the fact that work-at-home is a cooperative agreement between the company and our employees.”
Since March 12, all office meetings have been virtual, Marx said, and additional employees have transitioned to work at home.
Passport Health Plan administers the state’s Medicaid benefits to more than 300,000 Kentuckians, a number likely to grow as unemployment reaches record levels in the state due to the pandemic.
Passport Health Plan President/CEO Scott Bowers said his 500-plus employees have had to become very resilient in the face of new challenges. A significant portion of employees worked in the Louisville office and the entire team has transitioned to telecommuting.
“If our mission is to improve health and quality of life of our members, trying to be collaborative and innovate in this tough time is really critical,” Bowers said.
The Department for Medicaid Services has managed care organization meetings twice a week to discuss what’s important to the governor’s administration and how they can support that, Bowers said. Reports are already emerging about increased eligibility for Medicaid, which leads to more volume and accountability for PHP but so far, the growth has been accommodated.
Technology driving info, telemedicine
As the virus—and misinformation about it—began to spread, hospital websites and their social media quickly became trusted public health resources about COVID-19 and technology is also being leveraged to expand telehealth options for patients.
“Baptist Health has trained more than 1,000 providers to conduct these virtual care visits,” Fullenlove said. “Additionally, we are using telehealth in our hospitals so physicians can see patients in isolation remotely, or even do consults between providers in different facilities or hospitals. This is especially important now with a surge of patients involving a highly communicable infectious disease.”
In March, UK HealthCare implemented telecare patient visits for most outpatient care clinics, Newman said.
“In just a few weeks, more than 11,000 visits were completed in 103 clinics and more than 18,600 telecare appointments had been scheduled for the month of April,” he said.
At Pikeville Medical Center, drive thru-lab work and in-vehicle check-ins have been initiated and additional 24/7 drive-thru pharmacy lanes added. To avoid waiting room crowding, a texting platform notifies patients who arrive for a clinic visit when it’s time to come inside to see a physician. A respiratory-health triage area launched as well as telemedicine services.
Colvin communicates daily with St. Elizabeth hospital staff about the latest developments, and weekly with the Northern Kentucky legislative caucus and four area judge-executives. He also keeps in touch with nearby mayors and city administrators about the hospital’s ongoing efforts.
Researching treatment innovations
Meanwhile, Kentucky-based researchers, faculty and physicians are also busy working on treatments for the deadly virus.
A multidisciplinary team of UK researchers and faculty are working with their peers worldwide in a workgroup called the COVID-19 Unified Research Experts Alliance team. Its focus is “advising COVID-19 patient care and clinical trials based on emerging research and potential treatment options,” Newman said.
On March 29, Baptist Health Lexington transfused donated plasma from a recovered COVID-19 patient into two patients who were critically ill with the virus. The premise is that antibodies in plasma from recovered patients may help those still battling the virus. The treatment was a first-of-its-kind partnership with the Kentucky Blood Center and was performed after FDA and institutional review board approvals.
A COVID-19 patient at Norton Healthcare in Louisville has become the first worldwide to participate in a clinical study examining whether selinexor, a low-dose oral cancer treatment, can also benefit COVID-19 patients.
And at UofL, researchers announced in late April that they have developed a technology that shows promise for blocking the novel coronavirus from infecting human cells, with a requested fast-tracking from the Food and Drug Administration.
Ongoing care
With so much of the focus being on the coronavirus, there has been a reluctance by some to seek necessary treatment for other ailments, fearing they’ll come into contact with COVID-19 patients or contaminated surfaces. UofL’s Miller said this poses a different type of health risk, as troubling symptoms or conditions may worsen and later require more serious care.
“We’re taking the right precautions to make sure we don’t cross-infect anybody” and have strict cleaning processes, he said. “Don’t be hesitant about coming to us.” ■
Shannon Clinton is a correspondent for The Lane Report. She can be reached at [email protected].




















Add Comment